How to Test for Insulin Resistance

Insulin resistance is a hot topic and for good reason. It’s estimated over 50% of adults have it, as well as up to 70% of women with PCOS. If you don’t know what insulin resistance is, you should! It’s a silent condition that can lead to prediabetes, diabetes and increased risk of heart disease. Could YOU have it? Insulin resistance is tricky to diagnose and is not picked up on the usual blood tests. But are there are as signs and symptoms – and some blood tests – that may indicate you have it. Read on to learn more about how to test for insulin resistance. And stay tuned for my blog post next week on how to reverse insulin resistance naturally.
You may note that PCOS is discussed a lot in this post. This is one of my specialties in my nutrition practice and the majority of women with PCOS have some degree of insulin resistance. However the info in this post applies to everyone who may be at risk for insulin resistance!
What is insulin resistance?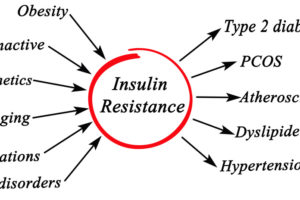
This topic was discussed last week in my long blog post. While the article was geared towards women with PCOS, I’d suggest you read it if this topic interests you. Here is a brief recap: eating a typical meal will cause glucose levels to rise. The more carbs you eat, especially if sugary or processed, the higher the blood sugar rises. Your body wants to get the blood sugar back down to a normal level. So the pancreas makes insulin, which tries to open the cell doors to get the sugar out of the blood and into the cells to be used for energy. However, in some people, the cells have become resistant to the insulin. Visualize a “key” getting stuck in the door and being unable to open it. The pancreas then has to secrete greater amounts of insulin to force the cells to take in the glucose. So now there are high levels of insulin in the blood. This makes the cells even more resistant to the insulin, so MORE insulin needs to be secreted. When the pancreas has to work really hard pumping out extra insulin for many years, it can eventually “wear out” and no longer produces enough insulin to get the blood sugar back to normal levels. This insulin resistant phase can last many years until it turns into prediabetes. In addition to increasing risk of prediabetes and diabetes, insulin resistance increases risk of heart disease.
What is the difference between type 2 diabetes and insulin resistance?
What many people don’t realize is that type 2 diabetes is a condition that takes many years to manifest. The body goes from functioning normally to  over secreting insulin in response to the cells not being sensitive to insulin —> pancreas not being able to make enough insulin to keep blood sugar in normal range (prediabetes) —> blood sugar gets more elevated (type 2 diabetes). Once diagnosed with prediabetes, you have a 50% chance of developing diabetes over the next 5-10 years unless you do something about it. The insulin resistance could have occurred for many years prior to diagnosis of prediabetes. Read my original blog post to find out why insulin resistance occurs.
over secreting insulin in response to the cells not being sensitive to insulin —> pancreas not being able to make enough insulin to keep blood sugar in normal range (prediabetes) —> blood sugar gets more elevated (type 2 diabetes). Once diagnosed with prediabetes, you have a 50% chance of developing diabetes over the next 5-10 years unless you do something about it. The insulin resistance could have occurred for many years prior to diagnosis of prediabetes. Read my original blog post to find out why insulin resistance occurs.
Stats on insulin resistance and prediabetes
Before I get into discussing how to diagnose insulin resistance, here are some stats:
- Nearly 50% of adults in the US have diabetes or prediabetes
- Over 1 in 3 adults have prediabetes (36% of all men and 29% of women) and only 11% know they have it
- Over 50% of those over age 65 have prediabetes
- Approximately 70% of women with PCOS have insulin resistance. 50% of women with PCOS will develop prediabetes or type 2 diabetes by age 40.
- Almost everyone with prediabetes or type 2 diabetes has some level of insulin resistance
- 66% of adults in the US are overweight or obese. Nearly everybody that is overweight is insulin resistant reference
So considering that 66% of adults are overweight or obese, it would seem that at least 60% of adults are insulin resistant to some degree (this is my “educated guess”!)
Tests to diagnose insulin resistance
Since insulin resistance usually has no symptoms, most people don’t know they have it. While doctors regularly perform blood tests (hopefully your doctor is doing this!) to check for diabetes and prediabetes, testing for insulin resistance isn’t commonly done. The main reason is that there aren’t many good tests. However, there are signs and symptoms that may indicate you have it. And you check for these yourself! And if you have PCOS, there are a few blood tests that may also indicate you have it … in addition to other tests that aren’t so useful. The best way to check for insulin resistance is a combination of a physical exam and certain blood tests.
–> Checklist for insulin resistance and metabolic syndrome
Insulin resistance is associated with a condition called Metabolic Syndrome. This is a constellation of symptoms including higher blood sugar, excess body fat around the abdomen, elevated cholesterol and high blood pressure. Here is a simple quiz to identify if you could possibly have it. 
The presence of 3 of the following 5 criteria means you have Metabolic Syndrome and are likely insulin resistant:
- Systolic blood pressure greater than 130 or diastolic blood pressure >85 or on treatment for hypertension.
- Central Obesity (more than 40 inches for men or 35 inches for women).
- Excess fat in the abdominal area can be dangerous compared to the fat on your hips, thighs and butt. This is because abdominal fat accumulates not only subcutaneously but also in internal organs such as the heart, pancreas, and liver, and in skeletal muscles (i.e.visceral fat), thus affecting their function. This fat releases active, hormone-like chemicals into the circulation. The majority of these are carried to the liver and contribute to fatty liver and insulin resistance.
- Fasting blood sugar greater than 100 mg/dl or on treatment for elevated blood sugar.
- Triglycerides >150 mg/dl or on treatment for elevated triglycerides.
- HDL cholesterol levels below 40 mg/dl for men or 50 for women.
–> Signs that you have may insulin resistance
Having several of the following may also be indicators of insulin resistance (the more signs, the greater the likelihood):
- You are middle-aged or older and overweight (especially in the abdominal area)
- Increased abdominal circumference with a waist measurement of 35 inches or greater for a woman and 40 inches or greater for a man
- Increased Waist-Hip Circumference Ratio is associated with abdominal obesity and insulin resistance. This test is even more accurate than the waist measurement alone. A diagnosis of abdominal obesity (android or visceral) is made if the waist-hip ratio (WHR) is equal to or higher than 0.8 in females, and equal to or higher than 1.0 in males. For example, if your waist is 32 and your hips are 35 —-> 32 divided by 35 = .91. This would indicate abdominal obesity. This can be helpful test
 that you can do on your own. And even if you are lean, high WHR levels are associated with insulin resistance markers.
that you can do on your own. And even if you are lean, high WHR levels are associated with insulin resistance markers. - Waist to height ratio (google to find online calculator). (ref Dr. Fiona)
<42 very slim
42-46: lean and healthy
46-49: healthy normal weight
> 50 increased risk for insulin resistance and type 2 diabetes - Acanthosis nigricans (dark velvety patches of skin behind the neck or under the arm)
- Skin tags
- Fatty liver
- Easy weight gain
- Difficulty losing weight
- PCOS
- Meeting 3 out of the 5 criteria as noted above
–> Blood tests for insulin resistance
Keep in mind that the typical tests for diabetes often don’t pick up insulin resistance. Nor does a fasting insulin. This is especially true in women who are mildly insulin resistance as well as women with “lean” PCOS. The following information was adapted from Dr. Fiona McCullough, PCOS expert. Download this handy chart to bring to your next doctor’s appointment. Even if you don’t have PCOS, the chart can be helpful.
BEST TESTS FOR DIABETES
Fasting glucose: done after an overnight fast.
Normal range is < 99 mg/dl (5.5 mmol/L) Glucose intolerance or prediabetes is 100-124. Over 124 is diabetes. Many individuals with insulin resistance have normal glucose
HbA1c: done anytime.
Normal range is < 5.7.
Interpretation: An HbA1c of 5.7-6.4 indicates pre-diabetes and 6.5 and higher is diabetes. According to the National Institute of Diabetes and Digestive and Kidney Diseases, if blood tests indicate prediabetes, insulin resistance most likely is present. However a normal test does not mean you are NOT insulin resistant!
C peptide: done after an overnight fast
C- peptide is not often tested except in those suspected of having type 1 diabetes however it can also be a surrogate marker of insulin resistance as levels can be higher than normal.
Normal values (fasting) : range from 0.51 – 2.72 ng/mL
Elevated levels suggest insulin resistance, however it is not diagnostic for insulin resistance.
Oral glucose tolerance test: done after an overnight fast at intervals over 2 hours after consuming 75 grams of glucose. *Note: if you follow a very low carb diet, you will need to consume extra carbs for 3 days prior to the test.
Normal range: glucose > 140 mg/dl (<7.8 mmol). Many patients with insulin resistance have completely normal glucose tolerance.
Interpretation:
- A 2 hour value between 140 and 200 mg/dL (7.8 and 11.1 mmol/L) is called impaired glucose tolerance. Your doctor may call this “pre-diabetes.” It means you are at increased risk of developing diabetes over time.
- A glucose level of 200 mg/dL (11.1 mmol/L) or higher is used to diagnose diabetes.
Fasting glucose/insulin ratio: This test is based on the results of 2 other lab tests, fasting glucose and fasting insulin.
Interpretation: a ratio < 4:5 suggests insulin resistance Reference: DR Futterweit
 TESTS FOR INSULIN RESISTANCE
TESTS FOR INSULIN RESISTANCE
Fasting insulin levels: done after an overnight fast.
Normal range is <8.4 ulU/ml (58 pmol/L) Note: many labs have normal values up to 30, however many experts feel the optimal insulin is considerably lower, usually considered to be </= 10.
Interpretation: May not pick up mild or moderate insulin resistance. Elevated levels suggest insulin resistance.
HOMA2: done after an overnight fast
Normal ranges: < 1.5 Ratio between fasting glucose and insulin. See the HOMA2 calculator here
Interpretation: > 3 significantly insulin resistant, >2 moderately insulin resistant
Triglyceride to HDL Ratio
A TG:HDL ratio >2.0–3.0 may indicate insulin resistance and metabolic risk.
Example: Triglycerides 150 / HDL 40 = 3.75 → elevated
BEST TEST FOR INSULIN RESISTANCE:
Hyperinsulinemic-euglycemic clamp is the gold standard for testing for insulin resistance. This is a complex lab procedure involving infusions of insulin and glucose, lasting 1-3 hours. However, it’s only done in research studies. So forget that one!
Oral Glucose Tolerance Test with Insulin: This is the 2nd best way to check for insulin resistance. It’s done after an overnight fast. Samples taken over either 2 or 4 hours at intervals after consuming 75 gm glucose. *Note: if you follow a very low carb diet, you will need to consume extra carbs for 3 days prior to the test.
Interpretation: Read Dr. Fiona’s article to get the response patterns! Patterns in increasing order of severity of insulin resistance and/or diabetes. Low levels of glucose during the test indicate reactive hypoglycemia particularly after 1-4 hours. This test is especially important for lean women with PCOS as they tend to have normal blood sugar and fasting insulin. It’s the post meal insulin that tends to the be the problem.
According to the AE-PCOS Society, an oral glucose tolerance test should be performed in all obese women, as well as in lean PCOS women with advanced age (> 40 years), in the presence of a personal history of gestational diabetes or family history of Type 2 diabetes.
Use signs and symptoms as noted above. If you can’t get this blood test done, then try the waist-hip ratio, check for the signs and symptoms mentioned above (abdominal obesity, skin tags, dark patches of skin, meeting 3 out of the 5 criteria for the metabolic syndrome). The Waist-Hip Circumference Ratio can also be helpful to suggest insulin resistance in lean women with PCOS.

Bottom line
Insulin resistance is the start of “something going wrong” with the metabolic processes in your body. If no changes are made, insulin resistance can lead to prediabetes, diabetes and increased your risk of heart disease. As a adult, there is a 50% chance you have it. And if you have PCOS, there is a 70% chance you have it (approximately). If you have PCOS, the best way to test for it is by the 2 hour glucose tolerance test with insulin levels, along with signs and symptoms. The good news is that there are many things you can do to decrease insulin resistance naturally! Stay tuned for my post next week on how to reverse insulin resistance naturally through diet, lifestyle and supplements (and medications if needed!)
Lastly, I am not providing medical advice on treating or diagnosing insulin resistance. This blog post is merely to give information on insulin resistance and talking points to discuss with your doctor. All medical conditions and treatments should be provided by your physician.
References:
How to Test for Insulin Resistance: Your Comprehensive Guide
Dr. Futterweit: A Patient’s Guide to PCOS: Understanding–and Reversing–Polycystic Ovary Syndrome
New CDC report: More than 100 million Americans have diabetes or prediabetes
Insulin Resistance: Risk Factor for Heart Disease and Diabetes
Early Detection of Insulin Resistance for Improved Patient Outcomes
RELATED POSTS
MEET MARTHA
I especially love problem-solving, whether it’s helping women defeat issues plaguing them for years, helping a busy executive find practical ways to get heart healthy, or providing tips to help you reverse diabetes. That’s why I’m on a constant quest to expand my knowledge by staying on top of the latest research.
3 Comments
Leave a Comment

20 Ways To Eat Out 550 Calories or Less!
No time to cook? We’ve got you covered. Here are 20 healthy meals from a variety of cuisines that won’t pack on the pounds. Most of them also have less than 30 grams of carbs.
Subscribe to my newsletter and get this free download.





My husband left me for another woman a few months ago and ever since then my life has been filled with pain and agony because my husband was my first love whom I have spent my entire life with. A friend and also a colleague from work told me he saw some testimonies of a spiritual counselor called Doctor Muna, He can bring back lover within some few days. Ridiculously, I laughed it out and said I am not interested. But for friendship’s sake, she consulted this God sent man on my behalf and to my greatest surprise, Immediately after 12 hours, my husband called me for the very first time for over 7 months saying “I miss you babe and I’m so sorry for everything I made you went through” I couldn’t say a word but cried over the phone and hanged up. We are back together and living Happily together again. To be honest, I still can’t believe it, because it’s highly unbelievable. Thank you DOCTOR MUNA for bringing back my love and also to my SELFLESS FRIEND. Laura, who interceded on my behalf. For anyone who might need help of this wonderful spiritual counselor, here is the email address: marvelspelltemple@gmail.com, Also add him on WhatsApp: +2347035449257
Wow what a good God I am so excited to tell you all how I become a millionaire I’m a woman of faith I was reading a comment on google where I meet a man sharing how Dr UYI cast a spell for him and he get his wife back after the spell I was interested I have to do research when I was doing the research I got so many testimony about this same man call Dr UYI how he help people to win lottery how he help people to get there ex back how he help people to do so many things I was happy and I contact him to help me win the lottery when I contact him and he told me what to do and after I did what he ask me to do he den gave me a lottery number to play and told me to go and buy ticket after playing the game I was so surprise the game come out good and I won the sum of 90, 000,000 dollars i was amazed and promise to share it to the people around me if anyone is willing to play the mage lottery it should contact Dr UYI so he can give you the right number to play thanks to you Dr UYI I’m so so grateful contact Dr UYI via drzukalottospelltemple@gmail.com OR WhatsApp on +17174154115
I was on holiday celebrating my 30th wedding anniversary when I received an email from the National Lottery to inform me that I had won, I never believed in voodoo spells until I became the winner of £61m EuroMillions Lottery with the winning numbers Chief Ade gave me with assurance that I was going to win, not every testimony you see online is fake, that was the same thing Chief Ade told me when I was doubting his spell before I finally agreed to give it a try. The purpose of my coming here is to let the world know that there are still real and genuine people on Earth, and Chief Ade is one of them. Are you struggling to win the lottery, or do you wish to win big on the lottery? Chief Ade is the way Email chiefadespellhome@gmail. com || WhatsApp +234 901 380 6328 THANK YOU ..