17 Diet and Lifestyle Tips to Decrease Inflammation

Inflammation is a hot topic these days – and for good reason! Chronic inflammation is linked to many diseases including heart disease, rheumatoid arthritis, Alzheimer’s, Parkinson’s, cancer, PCOS, inflammatory bowel disease and more. The typical American diet can cause inflammation. It’s rich in pro-inflammatory compounds, and low in antioxidants and other nutrients that help to prevent and control inflammation. And our lifestyle of too little sleep and exercise and too much stress and sitting time compounds our risk! The good news is that there are things we can do decrease inflammation as well as improve overall health and future health risks. Read on to get my top 15 diet and lifestyle tips to decrease inflammation.
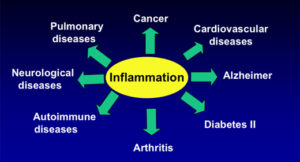
What is inflammation?
First, not all inflammation is bad. There are 2 main types: acute and chronic.
-Acute inflammation in the body helps us defend against bacteria and repair damaged tissues. It tends to have a rapid onset and be short lived. For example, when you cut your finger, it gets warm, red and swollen. This “inflammatory cascade” triggered by your immune system is your body’s attempt to heal itself. Once the threat has been taken care of, the inflammatory response shuts off.
Causes: infections, tissue damage, foreign bodies, hypersensitivity, autoimmunity
-Chronic inflammation can last months or years. It may occur with no apparent injury or disease, yet it may play a causative role in numerous diseases. As per Dr. Susan Blum, MD, MPH, author of The Immune System Recovery Plan, “Think of inflammation as irritating chemicals that are released by your immune cells. If this occurs in an ongoing way, damage occurs, and health problems can show up in any part of the body”. Chronic inflammation is linked to obesity and insulin resistance, cardiovascular disease metabolic syndrome, NAFLD (non-alcoholic fatty liver disease), psoriasis, inflammatory bowel disease, rheumatoid arthritis – to name a few.
Causes: genetics, environment, lifestyle, diet
 Markers of inflammation in the blood
Markers of inflammation in the blood
So how do you know if there is an inflammatory process going on in the body? One way is to test inflammatory markers in the blood. Inflammatory markers which may be increased include C-reactive protein, interleukin-18, monocyte chemoattractant protein-1 and white blood cell count. Other labs include: ESR – erythrocyte sedimentation rate, adiponectin, monocyte chemoattractant protein 1 (MCP-1), CD40 ligand lipoprotein-associated phospholipase A (2) (Lp-PLA(2)) , platelets and albumin (decreased albumin may indication inflammation). People who are obese and insulin resistant tend to have higher inflammatory markers, but even lean people can have elevated inflammatory markers due to medical conditions or lifestyle habits. Of note: the inflammatory process may be going on in the body even before these markers are elevated.
Diet and lifestyle tips to decrease inflammation
Lifestyle factors such as stress, inadequate exercise, lack of sleep and the typical Western diet rich in meat, sugar and refined carbs can all contribute to chronic inflammation. But keep in mind that the relationship between specific foods and increased inflammatory markers is unclear. The bottom line is that there are associations, but not causations. However, it’s likely that dietary/lifestyle patterns may be inflammatory or anti-inflammatory. Now does this mean that eating a cheese burger will cause your inflammatory markers to rise? Probably not (but your triglycerides and free fatty acids may!) But if you consistently follow consume the typical Western diet, along with poor lifestyle habits, it’s quite possible you’ll see an increase in inflammatory markers. A possible exception is for food sensitivities. I’ve had clients who were sensitive to certain foods immediately feel symptoms.
Here are my top 17 diet and lifestyle tips to decrease inflammation.
 Limit sugary foods and beverages as well as refined carbohydrates and grains, such as white bread and pastries and other highly processed and fast foods. The American Journal of Clinical Nutrition warns that processed sugars trigger the release of inflammatory messengers called cytokines. High-glycemic index foods also fuel the production of advanced glycation end (AGE) products that stimulate inflammation.
Limit sugary foods and beverages as well as refined carbohydrates and grains, such as white bread and pastries and other highly processed and fast foods. The American Journal of Clinical Nutrition warns that processed sugars trigger the release of inflammatory messengers called cytokines. High-glycemic index foods also fuel the production of advanced glycation end (AGE) products that stimulate inflammation.- Choose slow-digesting carbs found in vegetables, legumes, fruits and whole grains. They are good sources of fiber, fatty acid composition, magnesium, carotenoids, and flavonoids.
- Follow an anti-inflammatory diet. A traditional Mediterranean dietary pattern, which contains an abundance of fruits, vegetables, legumes, whole grains and a high ratio of monounsaturated (MUFA) to saturated (SFA) fats and omega 3 to omega 6 polyunsaturated fatty acid (PUFAs) and has shown anti-inflammatory effects when compared with typical North American and Northern European dietary patterns in most observational and interventional studies. Most experts believe that the Mediterranean diet is the diet of choice for diminishing chronic inflammation in clinical practice. Study. The following foods are part of the Mediterranean diet:
 -Omega 3 fats found in fatty fish like salmon (wild if possible), sardines, and herring. Walnuts, flaxseed, omega enriched eggs provide smaller amounts of omega 3 (a plant form called alpha-linolenic acid). The fats we eat are converted into substances called prostaglandins. Different types of prostaglandins ether increase or decrease inflammation in your body. Consuming foods rich in omega 3 fats help decrease the production of inflammatory prostaglandins
-Omega 3 fats found in fatty fish like salmon (wild if possible), sardines, and herring. Walnuts, flaxseed, omega enriched eggs provide smaller amounts of omega 3 (a plant form called alpha-linolenic acid). The fats we eat are converted into substances called prostaglandins. Different types of prostaglandins ether increase or decrease inflammation in your body. Consuming foods rich in omega 3 fats help decrease the production of inflammatory prostaglandins– Olive oil is rich in monounsaturated fat as well as polyphenols and antioxidants.
-Green leafy vegetables including kale, spinach, collard greens and Swiss chard contain powerful antioxidants, flavonoids, carotenoids, and vitamin C—all of which help protect against cellular damage. Ideally, opt for organic locally grown veggies that are in season. Make half your plate vegetables
-Spices including turmeric, ginger, garlic, basil, cayenne pepper, rosemary, sage, nutmeg, oregano, and thyme. They have been shown to have anti-inflammatory properties
 -Fruits such as strawberries, blueberries, cherries, and oranges are high in natural antioxidants and polyphenol (protective compounds found in plants) with anti-inflammatory effects
-Fruits such as strawberries, blueberries, cherries, and oranges are high in natural antioxidants and polyphenol (protective compounds found in plants) with anti-inflammatory effects -Green tea – researchers from the Laura W. Bush Institute for Women’s Health at the Texas Tech University Health Sciences Center found that regular green tea drinking enhances bone health and reduces inflammation in postmenopausal women
- Avoid excesses of omega 6 fats, prevalent in refined vegetable oils, such as corn and soy. Excess consumption of omega-6s can trigger the body to produce pro-inflammatory chemicals. These fatty acids are found in oils such corn, safflower, sunflower, grapeseed, soy, peanut, and vegetable; mayonnaise; and many salad dressings
- Avoid partially hydrogenated oils/trans fats, such as those found in some stick margarines, fried foods. prepackaged baked goods, flavored coffee creams (liquid and powder), some brands of shelf-stable peanut butter, and chocolate- or yogurt-coated snacks. Look for partially hydrogenated oils in the ingredient labels – and stay away!
 Limit fried and charred foods, which are high in advanced glycation end products (AGEs). Dietary AGEs are pathologic substances that have been implicated in the development and progression of various metabolic and chronic diseases. As the warm weather approaches, be careful not to get your meat too charred on the grill. Using an acidic marinade can help decrease AGE’s as can cooking over lower heat.
Limit fried and charred foods, which are high in advanced glycation end products (AGEs). Dietary AGEs are pathologic substances that have been implicated in the development and progression of various metabolic and chronic diseases. As the warm weather approaches, be careful not to get your meat too charred on the grill. Using an acidic marinade can help decrease AGE’s as can cooking over lower heat.- Limit red meat (burgers, steaks) and processed meat (hot dogs, sausage) as they tend to be inflammatory, especially in women, and those with obesity.Reference
- Individual food sensitivities may trigger an immune-based reaction which can lead to inflammation. Common allergens like casein and gluten (proteins found in dairy and wheat) are quick to spark the inflammatory cascade. Sensitivities are complex non-allergic, non-celiac inflammatory reactions that can involve both innate and adaptive immune pathways. A variety of triggering mechanisms trigger reactions in various types of white cells leading to the release of proinflammatory and proalgesic mediators, such as cytokines, leukotrienes, and prostaglandins. Mediator release and cellular reactivity ultimately results in subclinical and clinical inflammatory effects manifesting in a variety of clinical conditions and symptoms. If you think you might have a food sensitivity, consider getting food sensitivity testing done. You can also test one food at a time by omitting it for a few weeks to see if you notice an improvement. Then add it back in to see if you get symptoms.
 Eat foods good for the gut, including fermented vegetables and traditionally cultured foods. Optimizing your gut flora is important for a well-functioning immune system and helps ward off chronic inflammation. It’s believed that the majority of inflammatory diseases start in your gut, as in the result of an imbalanced microbiome. Fermented foods such as kefir, natto, kimchee, miso, tempeh, pickles, sauerkraut, olives, and other fermented vegetables, will help ‘reseed’ your gut with beneficial bacteria
Eat foods good for the gut, including fermented vegetables and traditionally cultured foods. Optimizing your gut flora is important for a well-functioning immune system and helps ward off chronic inflammation. It’s believed that the majority of inflammatory diseases start in your gut, as in the result of an imbalanced microbiome. Fermented foods such as kefir, natto, kimchee, miso, tempeh, pickles, sauerkraut, olives, and other fermented vegetables, will help ‘reseed’ your gut with beneficial bacteria- Lose weight if overweight. Even losing 5% of weight will decrease inflammatory markers
- Get adequate sleep. Scientists at Emory University School of Medicine in Atlanta, Georgia, found in a study that sleep deprivation or poor sleep quality raises inflammation, which in turn increases the risk of developing heart disease and stroke.
-
 Stress management. Chronic stress increases cortisol which directly influences your insulin levels and metabolism. It also plays a role in chronic inflammation and your immune system. Well-documented research links depression and stress to a rise in the inflammatory markers, such as CRP, signaling an increased risk for atherosclerosis and coronary heart disease (CHD). One study showed that a depressive state increases the odds of developing CHD by 50%. Read my blog post on dietary tips to manage stress.
Stress management. Chronic stress increases cortisol which directly influences your insulin levels and metabolism. It also plays a role in chronic inflammation and your immune system. Well-documented research links depression and stress to a rise in the inflammatory markers, such as CRP, signaling an increased risk for atherosclerosis and coronary heart disease (CHD). One study showed that a depressive state increases the odds of developing CHD by 50%. Read my blog post on dietary tips to manage stress. - Quit smoking if you smoke. Not much else to say on this one
- Sit less. Spending a lot of time sitting – even if you exercise on a regular basis – is associated with increased inflammatory markers (fasting insulin, leptin, leptin/adiponectin ratio, CRP, and IL-6), chronic low-grade inflammation and poor metabolic health. These effects have been shown in women more than men! Study
- Exercise on a regular basis – but don’t overdo it! While exercise in moderation plays an important role in decreasing inflammatory markers, going overboard can have the opposite effect. I’ve often had clients workout 2 hours a day 5-7 days a week in attempts to lose weight. This can do more harm than good. Moderate exercise at lower intensities is the better course. According to most studies, exercising under the 70% effort level seems to be the baseline for reducing inflammation and stress hormone levels. Moderate exercise efforts for up to 60 minutes can reduce inflammatory markers, increase positive neurotransmitters (e.g., serotonin and endorphins) and improve brain chemistry. Moderate intensities also stimulate the growth of new brain cells, neurons and capillary growth to muscles and neurons. Now this doesn’t mean you can’t throw a few intense HIIT sessions or some long cardio sessions into your workouts … just avoid the “more is better attitude”when it comes to exercise.
- Work on decreasing insulin levels if insulin resistant. High levels of insulin is linked to increased inflammation.
- Bonus: dark chocolate and red wine (in moderation) have been shown to have anti-inflammatory effects!
What habits do you have that are “inflammatory” or “anti-inflammatory”?
References
Women to Women. Causes of Inflammation.
Self-Reported Sitting Time and Markers of Inflammation, Insulin Resistance, and Adiposity
Diet and Inflammation
Exercise and the Inflammation Process
Dietitian Central continuing education course: Can Food Promote or Prevent Inflammation (dietitians can purchase this course to obtain credits)
RELATED POSTS
MEET MARTHA
I especially love problem-solving, whether it’s helping women defeat issues plaguing them for years, helping a busy executive find practical ways to get heart healthy, or providing tips to help you reverse diabetes. That’s why I’m on a constant quest to expand my knowledge by staying on top of the latest research.

20 Ways To Eat Out 550 Calories or Less!
No time to cook? We’ve got you covered. Here are 20 healthy meals from a variety of cuisines that won’t pack on the pounds. Most of them also have less than 30 grams of carbs.
Subscribe to my newsletter and get this free download.